 |
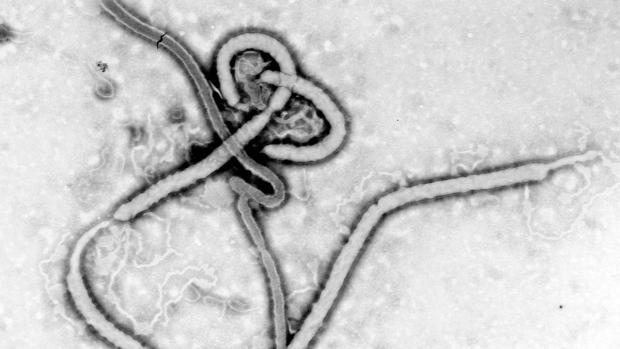
| A transmission electron micrograph shows the ultrastructural morphology displayed by an Ebola virus virion. (Centers for Disease Control and Prevention) |
A man who recently travelled to Sierra Leone walked into a southern Ontario hospital last week, feeling unwell. Four minutes later, he was in quarantine and being tested for the Ebola virus. Those tests on the patient in Belleville proved negative.
Suppose they'd been positive. What would happen next?
It would start with a technician at the National Microbiology Laboratory in Winnipeg, where the testing takes place, who would notify Dr. Gary Kobinger, the lab's chief of special pathogens, of the results.
Kobinger would double-check the sample. Once satisfied it was indeed positive, he would advise Steven Guercio, acting head of the laboratory.
Guercio would then notify four key people: Canada's new chief public health officer, Dr. Gregory Taylor; Krista Duthwaite, associate deputy minister of the Public Health Agency of Canada; Judith Bosse, assistant deputy minister of the agency's infectious disease prevention and control branch; and Theresa Tam, head of the agency's health security infrastructure branch.
Finally, Taylor and Outhwaite would notify federal Health Minister Rona Ambrose that Canada had its first confirmed case of Ebola.
The phone in Dr. David Mowat's office, meanwhile, would be ringing off the hook. Mowat, Ontario's interim chief medical officer of health, would get calls from everywhere: the local medical officer of health, the laboratory, Public Health Ontario, the hospital and the infectious disease doctor.
"If it's two o'clock in the morning, they will test it at two o'clock in the morning," Mowat said in an interview. "They'll have the results at three o'clock in the morning. They will call right then. For Ebola, that's exactly how it works.
"We've had results in the middle of the night before now. Mercifully, they've been negative results, but we get them."
Those phone calls would set off a chain of events shaped by Canada's past experiences with infectious-disease outbreaks: SARS in 2003 and the swine-flu pandemic of 2009.
The Public Health Agency of Canada has two teams of public health experts and epidemiologists on standby in case a patient tests positive for Ebola -- one in Winnipeg and another in Ottawa.
Since Ottawa is closer to Belleville, that team would race to the hospital. They'd bring laboratory expertise to quickly confirm the diagnosis, and any needed supplies, such as masks, gloves and face shields.
They'd be responsible for the hands-on treatment of the patient, who would remain in quarantine.
Back in Ottawa, the agency would alert the World Health Organization. And Ambrose and Taylor would hold a news conference to notify Canadians and allay public fears. The hospital might also hold a news conference of its own.
After that, the agency would send out daily updates, much like it did in 2009.
The plan reflects preparations that have been underway for some time.
Last week, Ontario designated 10 hospitals across the province as referral centres to treat potential cases of Ebola because they already have sophisticated infection-control systems in place.
And starting this week, Ebola specimens will be tested at Public Health Ontario's provincial labs, allowing for faster test results.
Behind the scenes, Ambrose has been busy. She held a conference call last week with her provincial and territorial counterparts to ensure they are fully prepared to deal with the disease should it make an appearance in Canada.
The minister has also met with representatives of the national nurses' union, which has complained of inadequate personal protective gear, training and preparedness for nurses, who would be on the front lines.
Ambrose said she reassured the nurses that they have her full support and that the government is committed to ensuring they have everything they need to feel safe.
Meanwhile, in addition to $35 million already pledged to the World Health Organization, the UN and humanitarian aid groups working in the affected region, Ambrose announced another $30 million Friday for the containment effort. Canada has also donated up to $2.5 million worth of personal protective equipment.
PHAC has also sent two mobile labs to Sierra Leone. One of the lab teams is working with Medecins Sans Frontieres to provide rapid diagnosis; the other is helping to improve infection prevention and control procedures.
Those teams check in every day with officials in Canada to update them on the situation on the ground.
Canada has also offered to donate a Canadian-developed experimental vaccine, currently undergoing clinical trials, to the WHO.
No comments:
Post a Comment